On May 17th, the ICMR convened COVID-19 National Task Force dropped convalescent plasma therapy from its virus treatment protocol. The decision, it said, was based on multiple studies that have found little to no use of convalescent plasma in treating COVID-19. This comes close on the heels of a recent World Health Organization (WHO) announcement that there is still no evidence to suggest that the antiviral drug Remdesivir is useful in treating hospitalised COVID-19 patients.
While many doctors treating COVID patients say these announcements are leading to confusion and constricting the already limited treatment options available to them, others believe that this is bound to happen, as most existing drugs and therapeutic options are still experimental and will continue to evolve over time as we gain a better understanding of the virus and its behaviour.
“It is a new disease and we are still in the process of understanding its clinical features,” said Dr Rajib Das Gupta, Chairman, Social and Community medicine, JNU, New Delhi. “Besides, there are new mutant variants. Since it is a viral disease, there are a few definitive therapeutic options. So, countries are constantly adapting the new investigation and treatment protocols on the basis of emerging evidence.”
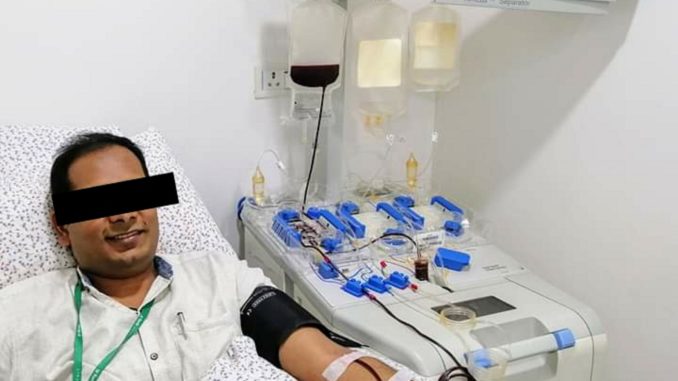
Convalescent Plasma Therapy (CPT), he points out, was initially seen to be effective. However, ICMR’s own PLACID trials in Sep 2020 found that there was no evidence that CPT was of any significant benefit. In May 2021, the RECOVERY trials in the UK also confirmed the conclusion.
No wonder then, over the past year, drugs such as Chloroquine, Remdesivir, Favipiravir and other experimental drugs, which were used in the treatment of COVID-19 across the globe, were later found to be of no or limited use.
“At times, we take decisions to use a drug or a therapy on the basis of clinical observation or a short-term clinical trial after reviewing the risks as well as benefits associated with it,” explained Dr Arun Kumar Sharma, a community medicine expert and director of NIIRNCD, an ICMR institute in Jodhpur. “But later if subsequent trials do not substantiate the initial findings, the decision can be reversed”.
For example, Chloroquine, which was introduced in the 1940s as an effective anti-malarial drug, was repurposed as a preventive drug in the case of COVID-19 after the Indian Council of Medical Research (ICMR) did a trial on healthcare workers. “As soon as healthcare workers started taking chloroquine as a prophylactic treatment, general people too believed that it could help protect them from getting the infection,” said Dr Sharma. “Sales went up manifold. But later it was found to be of not much use”.
Read more: Understanding Long COVID: The much-needed long term care you must be aware of
Similarly, Ivermectin, an anti-parasitic drug, which was largely used to lower the viral load in the initial phase of infection, was later dropped. “Safety and efficacy are important when using any drug for a new indication,” tweeted Soumya Swaminathan, WHO’s chief scientist. “WHO recommends against the use of ‘ivermectin’ for COVID-19 except within clinical trials,”.
Remdesivir, the much-in-demand drug in the treatment of moderate to severe COVID-19, which was hoarded and black-marketed till recently, has also been found to have limited role. “The fact is, a drug that specifically targets the coronavirus is still elusive,” says Dr N K Arora, a member of national COVID Task Force. “Many drugs which look very promising in the beginning have been seen in subsequent scientific studies to have little or doubtful value.”
No consensus among doctors
The medical fraternity is divided over such frequent changes in the treatment protocols. Many doctors believe that there are way too many guidelines issued by multiple regional, national and international institutions. Some doctors, who have used some of these drugs or therapy for their patients differ on whether or not these drugs should be dropped.
A transfusion medicine specialist from Lucknow said, on condition of anonymity, that he strongly feels convalescent plasma with good amount of antibodies has really helped in treating some of his patients who didn’t respond to other medicines. “The amount of antibodies in plasma varies from person to person,” said the specialist. “Plasma with low antibodies may not help but plasma from a person with high levels of antibodies can. What we should have done was to create a pool of donated plasma with enough antibodies in it.”
“Timing and the dosage of the drug makes all the difference when it comes to treating a COVID-19 patient,” pointed out Dr Rohit Bansal, a Singapore-based physician, who manages most of his patients with the help of medicines which have been in the treatment protocol at one time or another. “We need to have a proactive approach rather than a reactive approach. I keep a close watch on my patient’s vitals and prescribe the therapy accordingly. All the drugs be it Ivermectin or Remdesivir, play a crucial role in arresting the disease only when given at a specific stage — no sooner, no later”.
Dr Manisha Gupta, a Mohali-based internal medicine specialist agrees. “COVID-19 manifests in different severity in different patients,” explains Dr Gupta. “We tend to try everything possible when the patient is critical, especially if a therapy has helped some patients recover. But it is important to have some guidelines in place with a mechanism to update doctors on the ground. Also needed is a transparent, digital database where doctors can share their clinical observations with various drugs and therapies.”
Read more: Attack of the mutants: Will Sputnik help us in our COVID fight?
Though most doctors who have been treating COVID-19 patients have used various drugs and therapies at one point or the other, some feel that most of these drugs actually have a limited role to play. “Over the last one year I have observed that anticoagulants and steroids are the best drugs to treat moderate to severe COVID-19 patients,” observes Dr Nikhil Modi, who has been treating COVID-19 patients at Indraprastha Apollo Hospital, New Delhi. “However, the timing and dosage of these drugs are critical”.
Injudicious use of steroids can do more harm than good, adds Dr Himanshu Reddy, in-charge, COVID ward, KGMC, Lucknow. “Steroids if given too early in the treatment can worsen the case by facilitating viral multiplication in the body,” according to Dr Reddy. “And if given too much for too long a duration, steroids can make one susceptible to catching secondary bacterial and fungal infections such as mucormycosis. Similarly, drugs such as Tocilizumab can save some critically sick patients, but only when given in sterile settings. This drug is a strong immune suppressant and so should be used judiciously and only in specific situations as described by the ICMR”.
Read more: “Need a national registry on Black Fungus” – Dr Anant Bhan
Other possible drugs
Additions and deletions in the COVID-19 treatment guidelines will be a continuous process until a specific anti-COVID drug is developed. Other drugs such as Acalabrutinib, Baricitinib, Ruxolitinib, Tofacitinib, etc are also being tried and tested for COVID-19 treatment. Roche’s monoclonal antibodies—a cocktail of Casirivimab and Imdevimab—is also available to treat COVID patients India.
These are laboratory-made proteins that mimic the immune system’s ability to fight against the pathogens. These antibodies are specifically directed against the spike protein of SARS-CoV-2, the virus that causes COVID-19, and are designed to block the virus’ attachment and entry into human cells.
Approved for emergency use, these antibodies when given in the initial phase of the disease, can reduce the viral load in patients. In the US, these drugs are recommended for people with co-morbidities, compromised immune systems and patients highly susceptible to developing severe disease.
In the end, it is entirely up to the treating doctor to decide how and when to use a drug. “Any treatment cannot be robotic,” says Dr Arora. “There are decisions to be taken by a doctor on the spot depending upon his patient’s condition. Guidelines give a framework and help doctors understand the benefits and risks associated with various drugs and therapies. The bottom line is that they take an informed decision which is well within protocols”.
All about 2-DG, the new drug
(This information is based on a government press release. Citizen Matters was unable to get any independent comment from other doctors.)
An anti-COVID-19 2-deoxy-D-glucose (2-DG) has been developed by Institute of Nuclear Medicine and Allied Sciences (INMAS), a Defence Research and Development Organisation (DRDO) lab, in collaboration with Dr Reddy’s Laboratories (DRL), Hyderabad. Clinical trial results have shown that this molecule helps in faster recovery of hospitalised patients and reduces supplemental oxygen dependence. Higher proportion of COVID patients treated with 2-DG showed RT-PCR negative conversion.
In April 2020, during the first wave of the pandemic, INMAS-DRDO scientists conducted laboratory experiments with the help of Centre for Cellular and Molecular Biology (CCMB), Hyderabad and found that this 2-DG molecule works effectively against the virus and inhibits viral growth. Based on these results, the Drugs Controller General of India’s (DCGI) Central Drugs Standard Control Organization (CDSCO) permitted Phase-II clinical trials of 2-DG in COVID-19 patients in May 2020.
The DRDO, along with its industry partner DRL, started the clinical trials to test the safety and efficacy of the drug. In Phase-II trials (including dose ranging) conducted on 110 patients during May to October 2020, the drug was found to be safe in COVID-19 patients and showed significant improvement in their recovery. Phase- II-A was conducted in six hospitals and Phase-II-B (dose ranging) clinical trial was conducted at 11 hospitals all over the country.
In efficacy trends, the patients treated with 2-DG showed faster symptomatic cure than Standard of Care (SoC) on various endpoints. A significantly favourable trend (2.5 days difference) was seen in terms of the median time for achieving normalisation of parameters of specific vital signs when compared to SoC.
Based on successful results, DCGI further permitted Phase-III clinical trials in November 2020. This trial was conducted on 220 patients between December 2020 to March 2021 at 27 COVID hospitals in Delhi, Uttar Pradesh, West Bengal, Gujarat, Rajasthan, Maharashtra, Andhra Pradesh, Telangana, Karnataka and Tamil Nadu and detailed data of the clinical trial was presented to DCGI.
The data showed that patients who got the 2-DG drug showed a significantly higher proportion of improved symptomatically and became free from supplemental oxygen dependence (42% vs 31%) by Day-3 in comparison to SoC, indicating an early relief from Oxygen therapy/dependence.
A similar trend was observed in patients aged above 65 years. On May 1st, 2021, DCGI granted permission for Emergency Use of this drug as adjunct therapy in moderate to severe COVID-19 patients. Being a generic molecule and an analogue of glucose, it can be easily produced and made available in plenty.
The drug comes in powder form in a sachet, which is taken orally by dissolving it in water. It accumulates in the virus infected cells and prevents virus growth by stopping viral synthesis and energy production.
What makes this drug unique is its selective accumulation in virally infected cells.